Procedure/Surgery Name: Endovascular Glue Embolization of lower limb/leg Arterio-Venous Malformation (AVM)
Doctors: Dr. Bhavesh Arun Popat, Dr. Karan M Anandpara
Pre-Op Details & Diagnosis
A 29 year old female
- Progressively increasing painful swelling on anterior aspect of right distal leg of 4 months duration
- No skin changes
- Minimal right distal leg edema
- Tender on palpation +
- Distal pulses (ATA, DPA and PTA) palpable +
Investigation
- Local Ultrasound and Doppler – echogenic ill defined soft tissue area with few serpiginous vascular channels within s/o vascular malformation
- MRI – confirmed the findings of USG; arterial feeders with intralesional nidus noted s/o likely arterio-venous malformation (AVM)
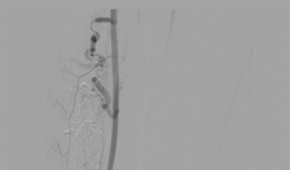
Angiography Findings:
- Abnormal leash of vessels
- Internal nidus
- Atleast 4 arterial feeders from anterior tibial artery
- Early draining vein – washout from accompanying anterior tibial veins
- Distal main anterior tibial artery and DPA shows slow, but antegrade adequate distal flow
Diagnosis
Complex arterio-veneous malformation (avm) of lower limb/leg with multiple arterial feeders from anterior tibial artery.
Treatment Plan
- Staged; combined ultrasound and fluoroscopic percutaneous and sos endovascular glue embolisation
- Followed by surgical excision
Procedure Details
- Percutaneous USG guided access taken
- Catheter in the right popliteal artery via left CFA access
- Endovascular contrast injection to localize the nidus and to monitor residual lesion
- Following this, multiple percutaneous access taken to target various components of the AVM
- Manual hand compression given to prevent inadvertent reflux into the draining vein
- Endovascular embolization attempted, but ultimately was not done due to high probability of reflux into the main anterior tibial artery due to intra-nidus vascular communication. Therefore, percutaneous embolization done with Glue
Post Procedure DSA
- Near complete exclusion of the AVM
- Glue cast visible
Conclusion
- Essential to classify vascular malformations appropriately – Venous, lymphatic, AVM, combined vascular malformations
- Set ‘realistic expectations’
- Multiple procedures
- Difficult to treat completely
- Team Work