
Deep vein thrombosis (DVT), as the name suggests, is a medical condition when a thrombus i.e a blood clot forms in the deep major veins of your body. Most commonly DVT occurs in the veins of the leg, but they can also occur in other parts of your body, including your arm, liver, brain, intestines, or kidney. But most commonly and as a generalization, DVT is usually associated with thrombosis involving the veins of your leg.
Vein are the vessels of the body carrying de-oxygenated blood from your periphery to the heart and lungs for purification. Arteries on the other hand carry good blood or oxygenated blood towards the periphery i.e. legs and other organs. These veins have valves carrying blood in only one direction. The pumping action of the muscles also assist in carrying blood. Two types of veins exist: the deep system called deep veins, and the superficial veins like the great and short saphenous veins. These superficial veins are an accessory system which assist in carrying the blood, but don’t play a major role. While the superficial veins can also get blocked and cause problems, it is the thrombosis of the deep veins which poses a major threat and is more concerning.
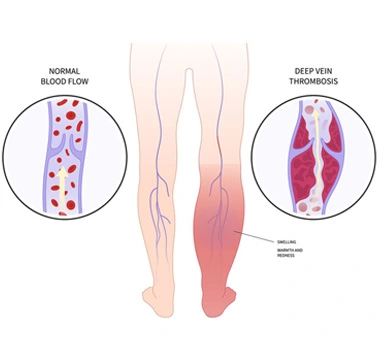
When these veins are either completely or partially blocked, blood gets stagnated and causes swelling. Due to this patient may develop lower limb pain, redness, swelling in the lower limbs. Rarely the blood clots may migrate to the heart or the arteries of the lung and cause risk to life as well. This is called pulmonary thromboembolism (PTE). Therefore, DVT can be dangerous if not diagnosed earlier and requires urgent attention and should not be ignored.
Deep vein thrombosis can have acute or short-term issues and long term issues. Therefore based on the time presentation DVT can be acute DVT (a-DVT) or chronic (long term DVT). Acute DVT is one that has occurred in the acute setting, where the clot has been formed in the first 14 days. Clots formed between 14 days to 1 month are called subacute DVT. Long standing (>1 month) remnant clots are called choric/long standing DVT.
Acute Deep Vein Thrombosis: Thrombus formed within the first month is called acute DVT. Acute DVT can cause acute sudden symptoms like leg redness, tenderness, swelling and pain. Sometimes, the swelling is so severe that the leg can become pale or blue due to blood pooling and blood stagnation. Rarely, an even worse symptom is compartment syndrome where the swelling is so severe that even arterial blood cannot reach the leg, this is a medical emergency.
The blood clots also have the ability to break free and travel through your bloodstream till your heart – this condition is called pulmonary thromboembolism (PTE/PE). Pulmonary embolism (PE) happens when the blood clots travel and get stuck in the blood vessels of your lung. Large clots may cause difficulty in breathing, drop of blood pressure or saturation. A quick diagnosis and treatment are needed, as this can be a life-threatening condition.
Chronic Deep Vein Thrombosis: Patient who have had DVT in the past (>1 month), which may or may not have been treated is called chronic DVT. About 50% of people who have DVT in their legs, will experience long term complications of DVT. Symptoms of chronic DVT may include cramping leg pain, swelling, pigmentation and recurrent ulcers affecting the quality of life. This is known as post-thrombotic syndrome (PTS) and may occur as a result of damage to the vein's inner lining and valves, which causes blood to accumulate more than it is supposed to. The affected leg is always hard, swollen and may show skin pigmentation and discolouration.
DVT occurs whenever blood gets stagnated in your legs for a long time, thus increasing your risk of thrombosis. DVT occurs based on something called the Virchow Triad i.e the blood is stagnant, hypercoagulable and there may be associated vessel wall injury. This predisposes to clotting following a triggering factor.
The following may contribute to increasing your risk of having deep vein thrombosis:
1. Inheriting the condition increases your risk of having blood clots. This is generally hereditary
2. Prolonged immobilisation
3. Facing cancer and its chemotherapy treatment
4. Family history of DVT
5. Recent Injury/trauma
6. Recent surgery, or immobility restrict the blood flow in a deep vein
7. Pregnancy
8. Consuming tobacco products like cigarettes, gutka, etc
9. History of varicose veins
10. Extreme dehydration
11. History of long travel causing standing or sitting in one place for a long time
What is the role of haematological testing in DVT
There are special tests requested to know if you have an underlying genetic condition predisposing to DVT. These tests include a panel of investigations to look for factor deficiencies in your blood. They cannot be done when you are on blood thinners since the results may be askew. Therefore, they are best done either before initiation or after 6-9 months, when anticoagulation can be stopped for a few days the clot is stable.
What is provoked versus unprovoked DVT?
Provoked DVT is when there is an underlying triggering factor that causes DVT for example history of prolonged immobilisation, dehydration or recent surgery. Unprovoked DVT is when there is no external triggering factor which has caused DVT. Unprovoked DVT is most likely due to an underlying genetic condition which causes the blood to be hypercoagulable.
Any other tests required for DVT management in the acute setting?
Routine blood tests will be ordered. A 2D echo will be asked for to look for pulmonary thromboembolism. If suspected, then a pulmonary angiography may be asked for. Creatinine levels may be requested, since these will be deranged. An ultrasound abdomen may be requested to look for a mass compressing the veins and causing DVT.
Chronic DVT is managed with compression stocking only. Acute DVT generally requires admission for monitoring. Patients need to be started on blood thinners or anticoagulants. Anticoagulants (blood thinners) make it harder for your blood to clot also stop clots from getting bigger and prevent blood clots from moving. The body has the ability to clear blood clots naturally but in some cases it doesn’t clear it totally.
Many types of anticoagulants are available in market like warfarin, heparin,etc. The doctor will suggest you the best possible medication for you. Oral form of anticoagulants like rivaroxaban and apixaban are now available. They need to be continued for upto 6-9 months. The treatment varies with each individual like if you had clots earlier, are you getting treatment for cancer and so on. The most common side effect of anticoagulants is bleeding. It is advised you connect with your doctor if you observe any injury or bleeding to avoid serious damages.
Recently newer treatment options like pharmacomechanical thrombectomy is available for acute DVT. This involves removing the entire clot from your veins using special devices and catheters. This should especially be promoted in young patients with acute/hyper-acute extensive DVT to prevent long term complications like post thrombotic syndrome. The exact details about the procedure, the management protocol is variable from case to case. Your doctor will best guide you for the correct treatment protocol for you.
